254 Everest Ln #3, St Johns, FL 32259
Tooth conditions can be assessed using quantitative measures. Fillings, root canals, or removals are determined based on three factors: how deep the infection travels, how the patient reacts to pain caused by a tooth, and what the x-ray or scan shows – not guessing. A correct diagnosis will prevent breakdown of the tooth structure, spread of infection to other systems, and repeat visits for the same issue.
All restorative options offered at Vitalize Dental in St. Johns are based on a structured diagnostic approach that combines endodontic principles (the study of dental pulp) with advanced diagnostic imaging techniques. The objective is to save as many healthy natural teeth as possible and eliminate infection at the point of origin.
The Core Difference: Surface Repair vs. Internal Infection Control
A dental filling becomes necessary when dental decay remains within the enamel and dentin layers. A root canal treatment (endodontic therapy) removes the pulp chamber and any infection that develops when bacteria reach the nerve tissue.
Attribute-Based Comparison
Infection Depth
- Filling: The dental filling procedure is performed when decay reaches only the enamel layer, which measures between 0.5 and 2 millimeters, or the dentin layer, which extends to about 3 millimeters.
- Root Canal: The infection has reached the pulp tissue, which contains nerve fibers and a blood circulation system.
Pain Duration
- Filling: The pain disappears within 15 seconds after the stimulus is removed.
- Root Canal: The pain persists for more than 30 seconds and occurs without any trigger.
Thermal Response
- Filling: Sensitivity triggered by cold or sweets.
- Root Canal: Heat sensitivity with lingering cold pain due to intrapulpal inflammation.
Diagnostic Signal
- Filling: Caries through bitewing radiographs, which display two-dimensional images.
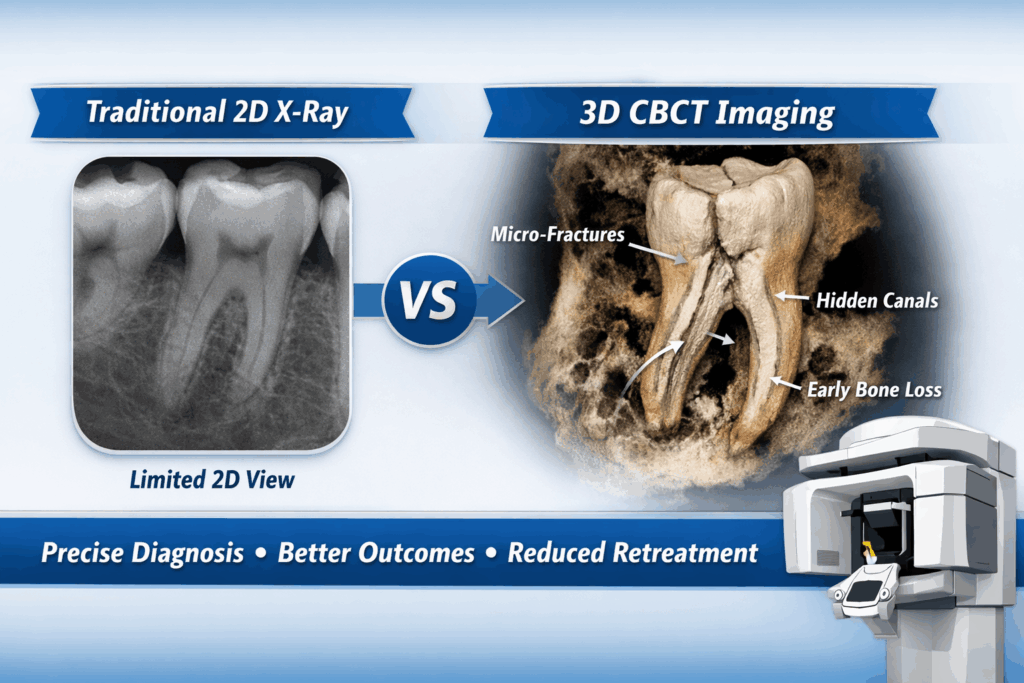
- Root Canal: The 3D CBCT imaging reveals periapical pathology through the appearance of apical radiolucency, which follows the root structure.
The Biological Threshold: When a Filling Fails as a Solution
A filling is an external seal of a tooth with external damage. However, it can not remove internal infections. Once bacteria invade the pulp, intrapulpal pressure increases, restricting blood flow and beginning necrosis. Therefore, if we seal this tooth now, we are trapping bacteria and accelerating the loss of bone around the root apex (tip) of the tooth.
This condition is classified as irreversible pulpitis, a defined pathological state—not a subjective symptom.
The 4 Critical Signs That Define the Need for a Root Canal
Each of these key signs represents a measurable biological change, and none of them overlap or are considered the same symptoms; they are all diagnostic thresholds.
1. Lingering Thermal Response
Direct Answer: Pain that lasts longer than 30 seconds after you have removed hot or cold stimuli means that a root canal is needed.
Expansion:
Thermal stimulation alters fluid movement inside dentinal tubules. In a healthy tooth, the response stops immediately when the stimulus is removed. In an infected pulp, inflammation increases internal pressure, resulting in refractory pain that persists even after the removal of the stimulus. This prolonged response confirms pulpal damage beyond reversible repair.
2. Spontaneous or Nocturnal Throbbing
Direct Answer: Pain that occurs spontaneously or without any external stimulus, particularly if it occurs at night, indicates that endodontic therapy is necessary due to irreversible pulpitis.
Expansion:
Blood flow to the head increases when lying supine, thereby increasing pressure in the inflamed pulp chamber (which has no room to expand) and generating a pulsating, throbbing sensation. Thus, this pulsating throb is due to the vascular congestion within the pulp and is not dependent on any external stimuli.
3. Referred Pain and Percussion Sensitivity
Direct Answer: The presence of pain that spreads to the jaw and ear, and nearby teeth, together with tooth sensitivity during tapping, signals that the infection has spread to the periodontal ligament.
Expansion:
The infection spreads from the root tip, damaging the bone and ligament tissues surrounding this area. The body develops apical periodontitis during this stage. The tooth develops vertical pressure sensitivity because the ligament tissue becomes inflamed. Referred pain occurs when different body parts share the same nerve pathways, although only one area shows symptoms.
4. Gingival Abscess
Direct Answer: A visible abscess or fistula on the gum confirms the need for a root canal to drain the infection.
Expansion:
A fistulous tract forms when infection creates a drainage pathway from the root apex to the gum surface. The parulis structure shows that an infection has become a long-term condition. The treatment requires more than antibiotics, as the infected pulp tissue must be removed to treat the disease.
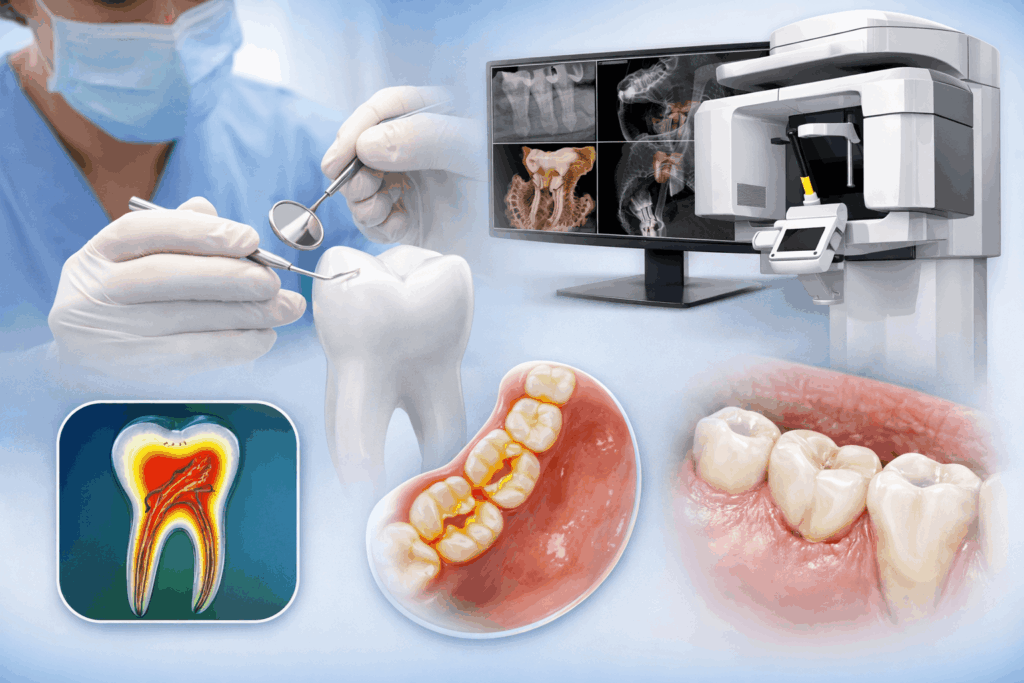
Diagnostic Precision: Why 3D Imaging Changes Outcomes
Traditional X-rays only give a 2D image of a tooth. They do not provide complete information about hidden infections and the complete root canal morphology.
At Vitalize Dental, we utilize 3D Cone Beam Computed Tomography (CBCT) to visualize the Z-axis depth of a tooth. This allows us to identify:
- Micro-fractures in roots
- Hidden accessory canals
- Early-stage bone loss not visible on 2D scans
By using this sophisticated technique to improve accuracy, we can help prevent incomplete treatment and subsequently decrease retreatment rates.
Structural Restoration After a Root Canal
After the infection is removed, the tooth loses moisture and internal structural integrity, which can increase the likelihood of fracture due to insufficient structural support from the loss of internal moisture.
A crown restores full function by distributing bite force evenly across the tooth.
Same-day dental crowns minimize the risk of the tooth fracturing upon return to biting by providing immediate protection and reducing this risk in the first 24 hours post-treatment.
The Timeline Difference: Filling vs. Root Canal
Dental Filling
- Procedure Time: 20–40 minutes
- Tooth Structure Removed: Minimal (decayed area only)
- Longevity: 5–10 years, depending on material and load
Root Canal + Crown
- Procedure Time: 60–120 minutes (can be same-day)
- Tooth Structure Removed: Internal pulp + infected dentin
- Longevity: 10–20+ years with proper crown placement
Local Care Rooted in Precision and Community
Located in the area of Durbin Park and Cimarrone, Vitalize Dental offers families advanced restorative dental treatment that is based on objective clinical evidence. At Vitalize Dental, each patient receives a diagnosis based solely on quantifiable data, not on generalized assumptions.
Dr. Neal Patel combines restorative dentistry with facial aesthetics. Each crown created after root canal therapy is designed to integrate with the patient’s bite and provide long-term stability and function.
The Diagnostic Entry Point
Each unique treatment begins with a dental examination assessment, which includes assessing:
- Pulp vitality
- Radiographic findings
- Occlusal stress patterns
- Periodontal condition
With early detection of disease or trauma, you will have less need for root canal therapy. When a diagnosis is delayed, structural compromise may occur due to the absence of treatment.
Preservation vs. Extraction: The Long-Term Perspective
A natural tooth maintains:
- Density of the jawbone, which is essential for maintaining healthy bone,
- Proper bite relationship, which is essential for a healthy jaw,
- Neurological feedback to your brain from the tooth when chewing.
Root canal therapy preserves these functions. Extraction removes them, often necessitating implants or bridges to restore biomechanical function.
Frequently Asked Questions
Yes. Removal of infected pulp eliminates the source of pressure and inflammation. Pain reduction begins within hours and stabilizes within 24–48 hours.
Yes. If decay progresses deeper into dentin and reaches the pulp, a previously filled tooth can require endodontic therapy.
Yes. Heat sensitivity indicates advanced pulpal inflammation and reduced blood flow regulation, which correlates with irreversible damage.
No. Antibiotics temporarily reduce the bacterial load but do not remove necrotic pulp tissue within the tooth. Infection persists without mechanical cleaning.
Pain lasting less than 15 seconds, sensitivity limited to cold, and the absence of spontaneous pain indicate reversible conditions treatable with fillings.
Related Articles
